Internal vs External Respiration: Understanding the Vital Gas Exchange Processes
Respiration is one of the most fundamental processes in living organisms, essential for survival and energy production. When we talk about respiration, many people immediately think about breathing—inhaling and exhaling air. However, respiration is far more complex and involves several distinct processes working in harmony. The two main types of respiration that occur in our bodies are internal respiration and external respiration. Understanding these processes helps us appreciate how our bodies efficiently extract oxygen from the air and deliver it to our cells while removing carbon dioxide waste.
What Is Respiration?
Before diving into the specifics of internal and external respiration, let's clarify what respiration actually means in a biological context. Respiration refers to the exchange of gases between an organism and its environment, as well as the cellular processes that use oxygen to break down nutrients and generate energy. This vital process ensures that all cells in the body receive the oxygen they need to function while eliminating the carbon dioxide produced as waste.
Have you ever wondered how oxygen from the air you breathe actually reaches each individual cell in your body? Or how the carbon dioxide produced by your cells makes its way out of your body? The answers lie in understanding the intricate mechanisms of internal and external respiration. These two distinct but complementary processes work together in a continuous cycle, sustaining life by maintaining proper gas exchange throughout the body.
The driving force behind both types of respiration is the partial pressure gradient of gases. Gases naturally move from areas of higher concentration (higher partial pressure) to areas of lower concentration (lower partial pressure) through diffusion. This simple principle is what makes both internal and external respiration possible without requiring energy expenditure for the actual gas exchange process.
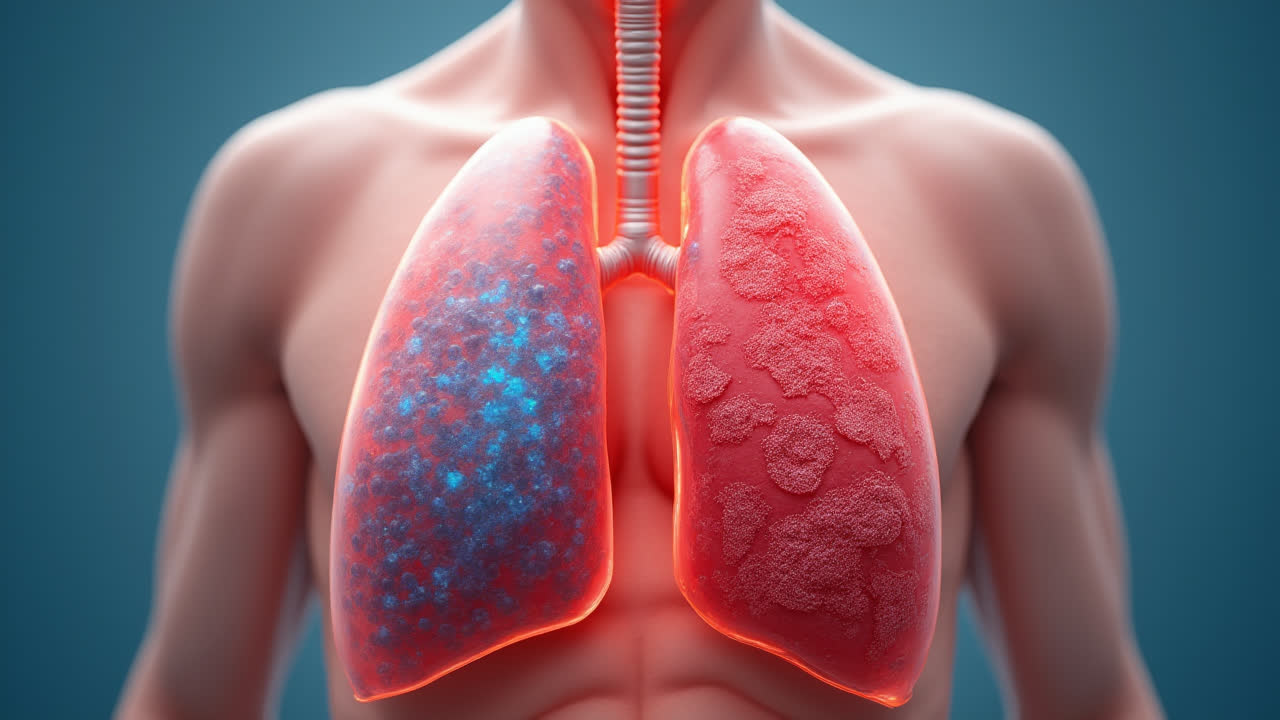
External Respiration: The Lung Exchange
External respiration refers to the gas exchange that occurs across the respiratory membrane in the lungs. When we inhale, oxygen-rich air enters the lungs and reaches tiny air sacs called alveoli. These alveoli are surrounded by capillaries—tiny blood vessels that carry deoxygenated blood. The walls of both the alveoli and capillaries are extremely thin, forming a respiratory membrane that allows gases to diffuse across easily.
In the lungs, the partial pressure of oxygen (PO₂) in the alveolar air is approximately 100 mmHg, while the PO₂ in the deoxygenated blood arriving from the tissues is only about 40 mmHg. This pressure gradient causes oxygen to diffuse from the alveolar air into the blood. Simultaneously, the partial pressure of carbon dioxide (PCO₂) in the blood is about 45 mmHg, higher than the PCO₂ in the alveolar air, which is around 40 mmHg. This causes carbon dioxide to diffuse from the blood into the alveolar air, which we then exhale.
After external respiration occurs, the blood leaving the lungs has a PO₂ of approximately 100 mmHg and a PCO₂ of about 40 mmHg. This oxygen-rich blood is then pumped by the heart to tissues throughout the body. The efficiency of external respiration can be affected by various factors, including lung diseases like emphysema or pulmonary fibrosis, which damage the respiratory membrane and impair gas exchange. That's why maintaining healthy lungs is crucial for optimal oxygen uptake and carbon dioxide removal.
One interesting aspect of external respiration is that it represents the interface between our internal environment and the external world. Through this process, elements from our surroundings—specifically, atmospheric oxygen—enter our bloodstream and become part of our internal environment. Similarly, waste products from our body's metabolism, in the form of carbon dioxide, exit our internal environment and are released into the atmosphere. This continuous exchange illustrates how intimately connected we are to our environment.
Internal Respiration: The Tissue Exchange
Internal respiration involves the exchange of gases between the blood and metabolizing tissues throughout the body. After oxygen-rich blood leaves the lungs, it travels through arteries to reach various tissues and organs. These tissues—particularly active ones like skeletal muscles during exercise—have a high demand for oxygen for cellular respiration, the process that produces ATP energy by metabolizing glucose.
In the tissues, the situation is reverse to what occurs in the lungs. The PO₂ in the blood is high (around 100 mmHg), while the PO₂ in the metabolizing tissue cells is low (approximately 40 mmHg) due to constant oxygen consumption. This gradient causes oxygen to diffuse from the blood into the tissue cells. At the same time, the PCO₂ in the tissue cells is high because carbon dioxide is continuously produced as a waste product of cellular respiration. The PCO₂ in the blood is lower, causing carbon dioxide to diffuse from the tissues into the blood.
After internal respiration takes place, the blood leaving the tissues has a decreased PO₂ (down to about 40 mmHg) and an increased PCO₂ (up to about 45 mmHg). This oxygen-depleted, carbon dioxide-rich blood then returns to the lungs via veins, where external respiration will occur again, completing the cycle. The efficiency of internal respiration can be affected by factors like blood flow to the tissues, the diffusion distance between capillaries and cells, and the metabolic rate of the tissue.
I've always found it fascinating how our bodies maintain this precise balance. Even when we increase our activity level—say, when running a marathon—our respiratory and circulatory systems adjust accordingly to ensure adequate oxygen delivery to the hard-working muscles. This remarkable adaptability highlights the sophistication of our body's gas exchange systems.
The Role of Hemoglobin in Respiration
Both internal and external respiration rely heavily on hemoglobin, the iron-containing protein found in red blood cells. Hemoglobin plays a crucial role in transporting both oxygen and carbon dioxide. When oxygen diffuses from the alveoli into the blood during external respiration, about 98% of it binds to hemoglobin, forming oxyhemoglobin. This binding greatly increases the blood's oxygen-carrying capacity—without hemoglobin, our blood would only be able to transport about 1.5% of the oxygen our cells need.
Hemoglobin's affinity for oxygen is influenced by several factors, including pH, temperature, and the concentration of carbon dioxide. In active tissues with high metabolic rates, the environment tends to be more acidic, warmer, and have higher levels of carbon dioxide. These conditions reduce hemoglobin's affinity for oxygen, facilitating the release of oxygen to the tissues that need it most—a phenomenon known as the Bohr effect.
Carbon dioxide transportation is also facilitated by hemoglobin. About 23% of carbon dioxide is transported as carbaminohemoglobin (carbon dioxide bound to hemoglobin). However, most carbon dioxide (about 70%) is transported as bicarbonate ions in the plasma, formed when carbon dioxide reacts with water in the presence of the enzyme carbonic anhydrase. The remaining 7% simply dissolves in the plasma. When blood reaches the lungs, these processes reverse, allowing carbon dioxide to be exhaled.
Comparative Analysis: Internal vs External Respiration
While both internal and external respiration involve gas exchange across respiratory membranes, they differ in several key aspects. Let's examine these differences in detail to gain a clearer understanding of these complementary processes.
| Characteristic | Internal Respiration | External Respiration |
|---|---|---|
| Location | Metabolizing tissues throughout the body | Lungs (alveoli) |
| Oxygen Exchange Direction | From blood into tissue cells | From alveolar air into blood |
| Carbon Dioxide Exchange Direction | From tissue cells into blood | From blood into alveolar air |
| Partial Pressure of Oxygen (PO₂) Change | Decreases from 100 mmHg to 40 mmHg | Increases from 40 mmHg to 100 mmHg |
| Partial Pressure of Carbon Dioxide (PCO₂) Change | Increases from 40 mmHg to 45 mmHg | Decreases from 45 mmHg to 40 mmHg |
| Blood Status After Process | Oxygen-depleted, CO₂-rich | Oxygen-rich, CO₂-depleted |
| Environmental Connection | Internal environment only | Connects internal and external environments |
| Primary Function | Delivers oxygen to cells for ATP production | Replenishes blood oxygen and removes CO₂ |
Clinical Implications of Respiration Disorders
Disorders affecting either internal or external respiration can have serious health consequences. Conditions that impair external respiration, such as pneumonia, asthma, or chronic obstructive pulmonary disease (COPD), reduce the efficiency of gas exchange in the lungs. This can lead to hypoxemia (low blood oxygen levels) and hypercapnia (elevated blood carbon dioxide levels), resulting in symptoms like shortness of breath, fatigue, and in severe cases, cyanosis (bluish discoloration of the skin).
Problems with internal respiration often involve issues with blood flow to tissues or cellular utilization of oxygen. Conditions like anemia reduce the blood's oxygen-carrying capacity due to decreased hemoglobin levels. Peripheral vascular disease limits blood flow to tissues, reducing oxygen delivery. Cyanide poisoning is an extreme example that directly interferes with cellular respiration by inhibiting the electron transport chain in mitochondria, preventing cells from using oxygen even when it's available.
Medical interventions for respiratory disorders often target specific aspects of internal or external respiration. Oxygen therapy increases the partial pressure of oxygen in inspired air, enhancing the pressure gradient for diffusion into the blood. Bronchodilators widen airways to improve ventilation in conditions like asthma. Erythropoietin treatment stimulates red blood cell production in certain types of anemia, increasing the blood's oxygen-carrying capacity.
Frequently Asked Questions About Respiration
What is the main difference between internal and external respiration?
The main difference between internal and external respiration lies in their location and direction of gas exchange. External respiration occurs in the lungs where oxygen moves from alveolar air into the bloodstream and carbon dioxide moves from the blood into the alveoli to be exhaled. Internal respiration happens at the tissue level where oxygen diffuses from the blood into tissue cells and carbon dioxide moves from the cells into the blood. These processes essentially work in opposite directions to maintain the continuous cycle of gas exchange necessary for cellular metabolism.
How do partial pressures drive the respiration process?
Partial pressures drive respiration through the principle of diffusion, where gases move from areas of higher concentration to areas of lower concentration. In the lungs, the partial pressure of oxygen (PO₂) in alveolar air is approximately 100 mmHg, while in deoxygenated blood it's only about 40 mmHg, causing oxygen to diffuse into the blood. For carbon dioxide, the partial pressure (PCO₂) is higher in the blood (45 mmHg) than in alveolar air (40 mmHg), so it diffuses out of the blood. This pressure gradient-driven process requires no energy expenditure for the actual gas exchange, making it highly efficient.
What role does hemoglobin play in the respiration process?
Hemoglobin plays a crucial role in respiration by significantly enhancing the blood's capacity to transport respiratory gases. About 98% of oxygen in the blood binds to hemoglobin, forming oxyhemoglobin, which dramatically increases oxygen-carrying capacity compared to simple dissolution in plasma. Hemoglobin also helps transport about 23% of carbon dioxide as carbaminohemoglobin. Additionally, hemoglobin's oxygen-binding affinity changes in response to tissue conditions—decreasing in areas with high metabolic activity (low pH, high temperature, high CO₂) through the Bohr effect, which facilitates oxygen release precisely where it's needed most.
Conclusion
Internal and external respiration represent two sides of the same physiological coin—complementary processes that together ensure the continuous exchange of gases necessary for cellular metabolism and life itself. External respiration in the lungs replenishes the blood's oxygen supply and removes carbon dioxide, while internal respiration delivers this oxygen to tissues and collects the carbon dioxide waste produced by cellular respiration.
The elegance of this system lies in its simplicity and efficiency. Driven by partial pressure gradients, gases naturally move from areas of higher concentration to areas of lower concentration without requiring energy expenditure for the diffusion process itself. The specialized structure of the respiratory membranes, the remarkable properties of hemoglobin, and the coordinated function of the respiratory and circulatory systems all work together to maintain this vital gas exchange.
Understanding the distinctions between internal and external respiration provides insight into how our bodies function at both the macro and micro levels. It also helps explain how various disorders can disrupt this delicate balance, leading to respiratory or metabolic problems. By appreciating these fundamental physiological processes, we gain a deeper understanding of our body's remarkable adaptability and the complex systems that sustain life with every breath we take.